You step off the curb, expecting your foot to land firmly, but instead, you stumble. Your arm wobbles as you reach for a glass. This unsettling lack of control is often described as coordination loss, medically known as Ataxia. It is not just clumsiness; it is a neurological sign caused by dysfunction in the Cerebellum or other pathways controlling motor movement. First systematically described by French neurologist Jean-Martin Charcot in 1868, this condition disrupts the precision timing of muscle commands. For millions living with it, understanding the difference between acute episodes and progressive forms is the first step toward managing daily life.
Understanding the Condition and Prevalence
Ataxia is characterized by impaired coordination of voluntary muscle movements. The cerebellum, which contains approximately 69 billion neurons-80% of the brain's total-is often the site of the issue. When damaged, it disrupts the smooth flow of information needed for balance and fine motor skills. According to the National Ataxia Foundation (2023), roughly 150,000 Americans are affected by various forms of this disorder. The most common hereditary type is Friedreich's Ataxia, affecting about 1 in 50,000 people.
Symptoms vary significantly based on the cause. Acquired ataxia can develop suddenly after a stroke or trauma, while hereditary forms appear gradually, often between ages five and twenty-five. Idiopathic late-onset cerebellar ataxia (ILOCA) typically emerges after age fifty with no clear cause. A 2020 European Journal of Neurology cohort study documented that gait instability is observed in 98% of cases, slurred speech (dysarthria) occurs in 92% of patients, and involuntary eye movements appear in 85%. These statistics highlight that the impact extends beyond walking stability to communication and vision.
The Reality of Neurological Rehabilitation
Many ask if therapy can reverse the damage. Current standard treatment focuses on symptom management rather than a cure. As evidenced by the 2022 American Academy of Neurology practice guidelines, no disease-modifying therapies exist for most ataxia types. However, this does not mean recovery is impossible. The primary value proposition of Neurological Rehabilitation lies in its capacity to improve functional independence and quality of life metrics. A 2021 Cochrane systematic review of 37 clinical trials involving 1,842 patients found that proper intervention improved quality of life by 25-40%.
| Therapy Type | Functional Improvement | Evidence Level |
|---|---|---|
| Task-Specific Training | 35% greater improvement | High (RCT) |
| Traditional Physical Therapy | Baseline standard | Moderate |
| Biofeedback Systems | 8.2 point increase (Berg Scale) | High (Mayo Clinic) |
Not all exercises work for everyone. Comparative analysis reveals that task-specific training demonstrates 35% greater functional improvement than traditional physical therapy approaches. This was shown in a 2022 head-to-head trial published in the Journal of Neurologic Physical Therapy. Conversely, constraint-induced movement therapy, which helps hemiparesis, actually worsens symptoms in 68% of ataxia patients due to the condition's different pathophysiology. This distinction is critical because using the wrong protocol can set progress back significantly.
Finding Specialized Care and Certification
A major barrier to progress is access to therapists who truly understand the condition. Generic therapy centers often lack specific expertise. In the United States, the CRED certification program, developed by the University of Alabama at Birmingham, requires 120 hours of specialized training. As of December 2023, they had certified 327 physical therapists. Despite this, significant access disparities exist. There is one certified therapist per 458 patients in rural areas versus one per 87 in urban centers.
Patient experiences documented across Ataxia UK's 2022 community survey reveal consistent patterns regarding care quality. Positive outcomes include improved walking stability (78% after 12 weeks of intensive therapy) and reduced fall frequency (from median 3.2 to 0.7 falls/week). However, negative experiences centered on therapy access barriers. 63% of respondents reported insurance denials for necessary sessions beyond arbitrary visit limits. One Reddit user noted paying $3,200 out-of-pocket when coverage stopped after 20 visits despite needing 40.
Implementation Phases and Protocols
Effective rehabilitation follows structured protocols. The 2022 International Ataxia Rehabilitation Guidelines outline a phased approach tailored to patient capability:
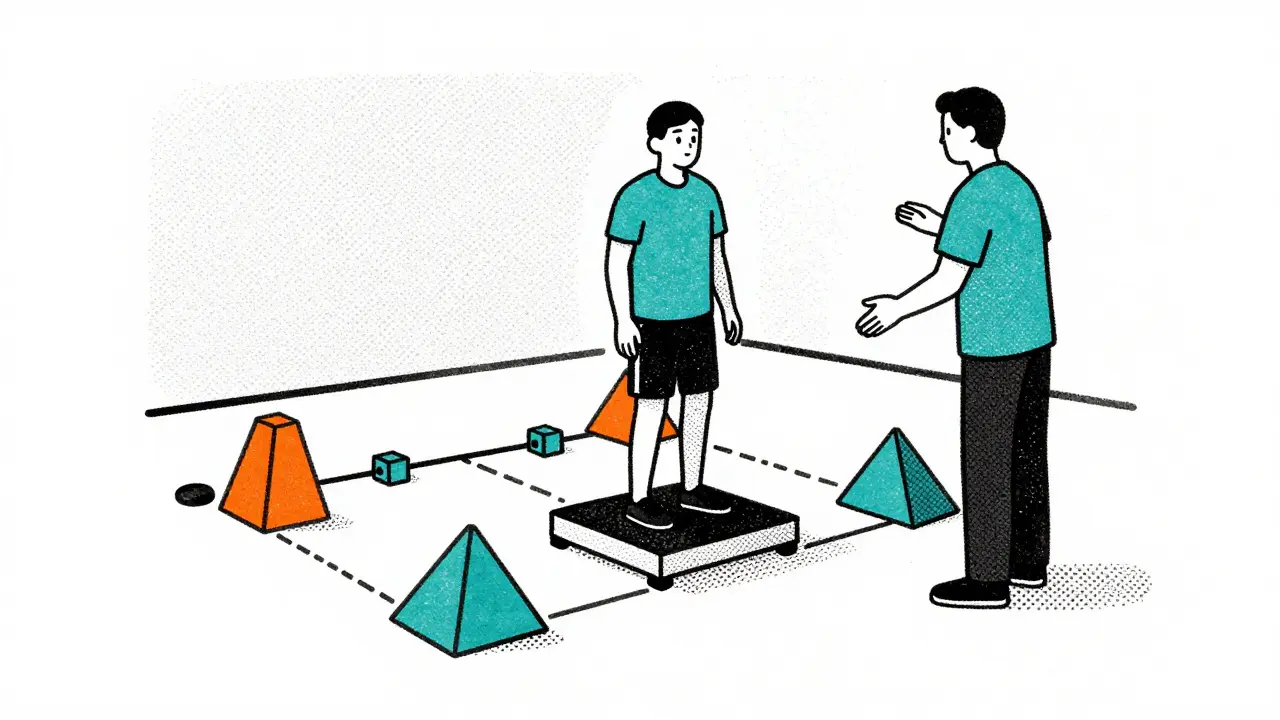
- Phase 1 (Weeks 1-4): Focuses on static balance training with dual-task challenges. Patients learn to stand still while performing cognitive tasks to build core stability.
- Phase 2 (Weeks 5-8): Incorporates dynamic gait training with obstacle negotiation. This introduces controlled movement over uneven surfaces.
- Phase 3 (Weeks 9-12): Emphasizes community ambulation and fall prevention. Skills learned in clinic are applied to real-world environments like shopping malls or busy streets.
Dr. Jeremy Schmahmann of Harvard Medical School emphasizes that "ataxia rehabilitation must address both motor and non-motor symptoms." About 70% of patients experience executive function deficits that impact therapy adherence. Therefore, successful programs integrate speech-language pathology interventions alongside physical movement. Standard sessions typically occur 3-5 times weekly for 60-90 minutes. Treatment costs range from $120-$250 per session in the United States, with Medicare covering approximately 65% for medically necessary care.
Technological Innovations and Future Trends
Technology is reshaping how we treat coordination loss. Balance training using computerized dynamic posturography systems, such as the NeuroCom SMART Balance Master, produces measurable improvements in Berg Balance Scale scores compared to conventional therapy. Robotics-assisted gait training shows promise in stroke rehabilitation but has limited efficacy for cerebellar ataxia, with only 12% of patients achieving clinically meaningful improvements.
New developments include the 2023 FDA clearance of the Cerebello wearable device developed by NeuroQore. It provides real-time tremor suppression through targeted neuromodulation, showing 32% improvement in upper limb function in pivotal trials. Additionally, emerging research on non-invasive brain stimulation techniques shows promise. Cerebellar transcranial direct current stimulation (ctDCS) combined with physical therapy produced 22% greater improvement in Scale for the Assessment and Rating of Ataxia (SARA) scores than therapy alone.
However, cost remains a hurdle. Advanced tools like virtual reality systems show 28% greater engagement than traditional therapy but are available at only 15% of comprehensive rehabilitation centers due to high costs ($120,000-$350,000 per system). The Ataxia Global Research Consortium is currently conducting a large rehabilitation trial testing intensive versus distributed practice schedules, with results expected in Q3 2025.
Financial Barriers and Coverage Realities
Navigating the financial landscape is often as difficult as the physical challenges. Medicare reimbursement rates for ataxia rehabilitation decreased by 7.3% from 2021-2023 due to fee schedule adjustments. Private insurance typically covers 60-80% of costs, resulting in average annual out-of-pocket expenses of $2,450 per patient. The Centers for Medicare & Medicaid Services have strict medical necessity requirements that often limit therapy to 10-20 visits regardless of documented progress.
This creates a tiered system of care. Academic medical centers provide 68% of specialized services, while community clinics often lack necessary expertise. Only 22% of community clinics have therapists with specific ataxia training according to the American Physical Therapy Association's 2022 workforce survey. Financial strain is significant; 31% of users report annual household incomes below $50,000, creating barriers to optimal care. Without policy changes addressing reimbursement limitations, access to evidence-based rehabilitation may deteriorate for 65% of patients by 2030.
Is ataxia curable?
There is currently no cure for most forms of ataxia. Treatment focuses on managing symptoms through multidisciplinary rehabilitation to improve functional independence and quality of life.
How effective is physical therapy for ataxia?
A 2021 Cochrane review suggests rehabilitation can improve quality of life metrics by 25-40%. Task-specific training shows 35% greater functional improvement compared to traditional methods.
What is the cost of ataxia rehabilitation?
Treatment costs range from $120-$250 per session in the US. Private insurance covers 60-80%, but average annual out-of-pocket expenses remain around $2,450 per patient.
Can technology help with balance?
Yes, systems like NeuroCom SMART Balance Master and wearable sensors show measurable improvements. Virtual reality systems have demonstrated 28% greater patient engagement than traditional therapy.
Where do I find a specialist?
Look for therapists with CRED certification. While scarce in rural areas (1 per 458 patients), urban centers have better ratios (1 per 87 patients). University hospitals often host specialized programs.


Amber Armstrong
Reading about ataxia always hits hard when you see the stats. It is really tough imagining the daily struggle with coordination loss. My cousin had something similar years ago and it changed everything for him. Seeing the numbers about gait instability makes sense because walking is so basic. We often forget how much effort goes into just standing upright sometimes. The part about insurance denials is absolutely heartbreaking to read honestly. People need therapy to function but money stops them dead in their tracks. Thirty-one percent of users making under fifty thousand dollars is a huge statistic. It feels wrong that healthcare depends so heavily on your bank account balance. I hope more people get access to those certified therapists mentioned in the table. Task-specific training sounds intense but also like the best possible option. Traditional PT seems insufficient compared to what these newer studies show. We need better support systems before we talk about curing anything entirely. Technology helps a lot but cost remains the biggest wall in front of progress. Keeping hope alive is essential while waiting for real systemic changes to arrive.