When you pick up a prescription at the pharmacy, you probably don’t think about why your insurer covers one generic drug but not another-even if they’re both the same medicine. But behind that simple decision is a complex system designed to save money, reduce risk, and keep patients on treatment. Insurers don’t just pick generics at random. They follow strict, evidence-based rules. And understanding how they work can help you avoid surprises and get the meds you need.
Generics Aren’t All Treated the Same
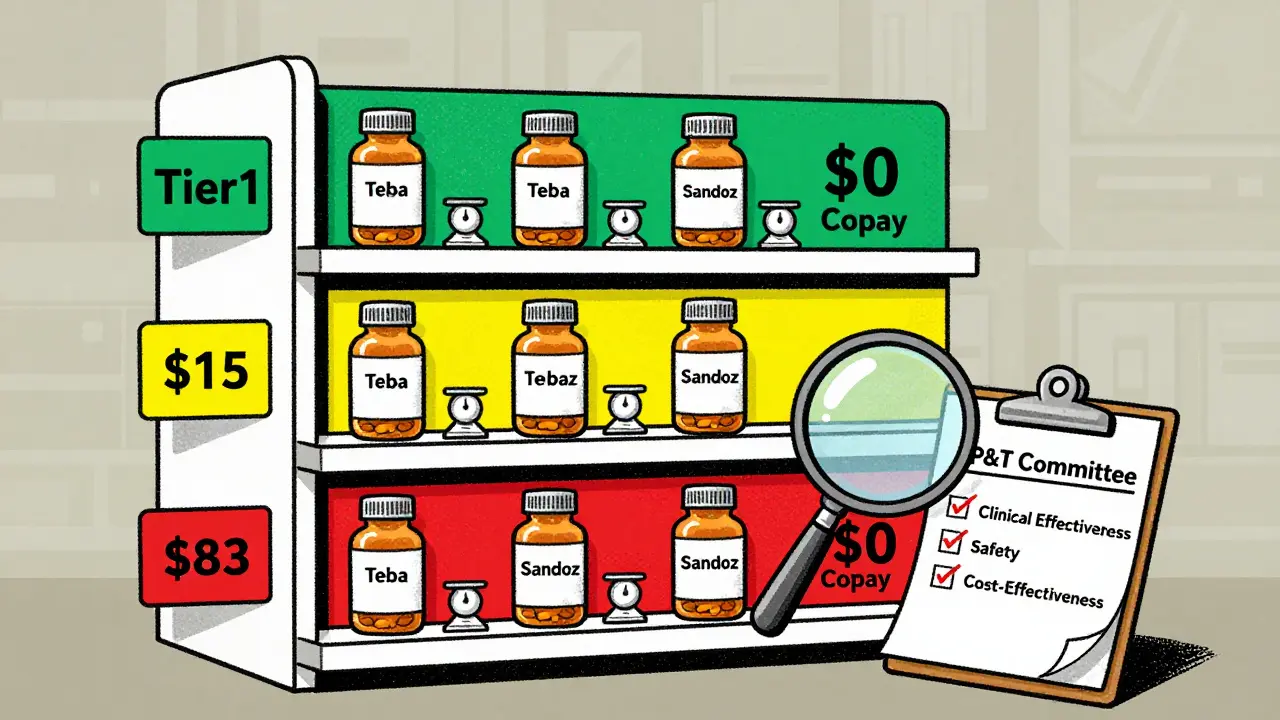
Not every generic drug gets the same treatment from your insurance plan. Some are covered with a $0 copay. Others might require a $15 payment. A few might not be covered at all. Why? It comes down to how insurers organize their formularies-lists of drugs they agree to pay for. Most plans use a tiered system, usually with 3 to 5 levels. Generics almost always land in Tier 1-the lowest cost tier. That’s because they cost 80-85% less than brand-name drugs. The FDA says generics must have the same active ingredient, strength, dosage, and route of administration as the brand. And they must be therapeutically equivalent, meaning they work the same way in your body. For example, if you’re prescribed a brand-name blood pressure pill, your insurer will likely cover a generic version of that same drug. But if there are two different generics available-one made by Teva and one by Sandoz-they might only cover the cheaper one. That’s not because one is better. It’s because the insurer negotiated a better price with one manufacturer.The Committee That Decides What Gets Covered
Every major insurer has a Pharmacy & Therapeutics (P&T) committee. These are groups of doctors, pharmacists, and sometimes patient advocates who review drugs and decide what goes on the formulary. They don’t just look at price. They look at three things:- Clinical effectiveness: Does the drug actually work? Are there studies showing it helps patients live longer, feel better, or avoid hospital stays?
- Safety: Does it cause more side effects than other options? Are there warnings from the FDA or real-world reports of problems?
- Cost-effectiveness: If two drugs work the same, but one costs half as much, the cheaper one wins.
Why Some Generics Are Excluded
You might wonder: if generics are all the same, why would one be left out? The answer is usually about timing or supply. New generics hit the market all the time. But insurers don’t rush to add them. They wait to see:- Is the manufacturer reliable? Have there been quality issues or recalls?
- Is the supply stable? The FDA reported 372 active drug shortages in late 2023, and 78% of them were generics. If a drug is hard to get, insurers avoid it.
- Is there a better alternative? If a newer generic has been shown to have fewer side effects, the older one might get bumped.

How Much You Pay Depends on the Tier
Your out-of-pocket cost for a generic isn’t random. It’s tied directly to its tier. Here’s what typical costs look like for a 30-day supply:| Tier | Drug Type | Typical Copay |
|---|---|---|
| Tier 1 | Preferred generics | $0-$10 |
| Tier 2 | Non-preferred generics | $10-$20 |
| Tier 3 | Brand-name drugs | $40-$100+ |
| Tier 4 | Specialty drugs | $100-$500+ |
What Happens When Your Drug Isn’t Covered
If your doctor prescribes a generic that’s not on your plan’s formulary, you’re not stuck. You can request an exception. This is common. The Patient Advocate Foundation found that 43% of patients get an initial denial-but 78% eventually get coverage after appealing. To win an exception, you or your doctor need to show one of these:- The covered generic caused side effects you didn’t have before
- You tried it and it didn’t work
- You need a higher dose than your plan allows

The Hidden Problem: Therapeutic Substitution
Here’s where things get tricky. Even if your doctor prescribes a specific generic, your pharmacy might swap it for another one that’s cheaper. This is called therapeutic substitution. It’s legal, and it’s common. About 78% of commercial insurance plans allow this. But it’s not always safe. A 2023 Drug Topics survey found that 31% of patients reported adverse effects after being switched to a different generic. Why? Because while the active ingredient is the same, the inactive ingredients-like fillers, dyes, or coatings-can vary. For some people, especially those with allergies or sensitivities, that’s enough to cause problems. If you’ve had a bad reaction to a switch, ask your doctor to write "Do Not Substitute" on the prescription. Most insurers will honor that.What’s Changing in 2025 and Beyond
The rules are shifting. The Inflation Reduction Act of 2022 capped out-of-pocket drug costs for Medicare Part D at $2,000 per year starting in 2025. That means insurers can’t just push patients toward the cheapest drug anymore. They have to think about total cost-not just the copay. Also, the FDA is speeding up approval of complex generics-like inhalers, insulin, and injectables. That could mean more options soon. But it also means more decisions for P&T committees. Right now, 62% of them say they’re unsure how to handle AI-driven personalized generics, which are just starting to appear. Meanwhile, the generic drug market is growing fast. It’s expected to hit $112.6 billion by 2027. But drug shortages remain a threat. If a manufacturer can’t keep up, insurers scramble to find replacements-and patients get caught in the middle.What You Can Do
You don’t have to be passive in this system. Here’s how to take control:- Ask your pharmacist: "Is this the preferred generic on my plan?" If not, ask if there’s a cheaper option.
- Call your insurer and ask for a copy of their formulary. Most have it online.
- If a drug isn’t covered, ask your doctor to file an exception. It’s easier than you think.
- Keep a list of any side effects you’ve had after switching generics. Bring it to appointments.
- Use mail-order pharmacies-they often have better pricing on generics.
Why do some generics cost more than others on my plan?
It’s not about quality-it’s about negotiation. Insurers strike deals with manufacturers for the lowest price. The cheapest option becomes the "preferred" generic. If you’re prescribed a more expensive version, you might pay more unless you get an exception. Always ask if there’s a lower-cost alternative.
Can my insurance force me to switch to a different generic?
Yes, if your plan allows therapeutic substitution. But your doctor can stop this by writing "Do Not Substitute" on the prescription. If you’ve had side effects from a switch before, make sure your doctor documents it. That gives you legal leverage to stay on the drug that works for you.
How long does it take to get a drug covered if it’s not on the formulary?
If your doctor files an exception request, insurers must respond within three business days. For urgent cases-like if you’re at risk of hospitalization-they must respond in one day. If they don’t answer on time, your request is automatically approved.
Are all generics really the same?
The active ingredient is identical. But the inactive ingredients-like binders, dyes, or coatings-can differ. For most people, that doesn’t matter. But for some, especially those with allergies, sensitivities, or complex conditions, switching generics can cause side effects. Always tell your doctor if you notice changes after a switch.
Will the Inflation Reduction Act change how insurers pick generics?
Yes. Starting in 2025, Medicare Part D patients won’t pay more than $2,000 a year out-of-pocket for drugs. That means insurers can’t rely on high copays to discourage use. They’ll likely focus more on volume and long-term outcomes-like keeping patients healthy enough to avoid hospital visits-rather than just picking the cheapest pill.

Joey Pearson
Love this breakdown! Seriously, most people have no idea how much power they have in this system. Just asking your pharmacist if there’s a cheaper generic can save you $50 a month. I did it last month and switched to a $0 copay version of my blood pressure med. No drama, no hassle. You’re not just a patient-you’re a consumer. Own it! 😊