When you pick up a prescription, you might assume all generics are cheap. But that’s not always true. Some generic drugs cost nearly as much as the brand-name version - and that’s where the real savings get hidden. The biggest opportunity to cut costs isn’t always in switching from brand to generic. It’s in switching from one generic to another - or better yet, from multiple individual generics to a single combination product.
Take asthma inhalers. For years, patients on Advair Diskus paid around $334 per inhaler. Then, in 2019, the first generic version, Wixela Inhub, hit the market. The price dropped to $115. That’s a 65.6% savings per inhaler. But here’s the twist: Advair Diskus was already a combination product - it combined two drugs in one device. Before generics, patients had to buy two separate inhalers, each with their own price tag. The combination wasn’t just convenient. It was cheaper.
That’s the pattern. Combination generics often beat the cost of buying the same drugs separately. A 2022 study found that switching from separate generic medications to a single combination version cut costs by an estimated $941 million per year in the U.S. alone. Why? Because manufacturing, packaging, and distribution costs are spread across one product instead of two. And when multiple generic makers compete to produce that single combo, prices plunge even further.
Why Some Generics Cost More Than Others
Not all generics are created equal. The FDA says a generic must be bioequivalent to the brand - meaning it works the same way in the body. But it doesn’t say anything about price. In fact, a 2022 analysis of Colorado’s pharmacy data found 45 high-cost generics that had cheaper alternatives with the exact same effect. These weren’t brand-name drugs. They were other generics. And they were, on average, 15.6 times cheaper.
One example: a 30-day supply of a generic blood pressure pill might cost $45. But a different generic version of the same drug - same active ingredient, same dose - costs $3. That’s a 93% drop. The difference? Competition. If only one company makes that $45 version, they can charge what they want. If five companies make the $3 version, prices crash.
Even more surprising: 62% of these high-cost generics could be replaced by a different strength or dosage form of the same drug. For instance, a tablet that costs $20 might be replaced by a capsule with the same dose that costs $1. Or a 30-pill bottle might be swapped for a 90-pill bottle - same total drug amount, but you pay less per pill because of bulk packaging.
Combination Drugs: The Hidden Savings Engine
Combination drugs - pills or inhalers that contain two or more active ingredients - are the unsung heroes of generic savings. They’re not new. But their impact on cost is still underused.
Think about diabetes. A patient might be prescribed metformin, sitagliptin, and glimepiride - three separate pills, each a generic. Each costs $10 to $15 a month. That’s $30 to $45 monthly. But now there’s a generic combo pill that includes all three. It costs $18. That’s a 50% savings just by switching.
Same with heart disease. A common combo is amlodipine and atorvastatin. Buying them separately? $20 and $12. The combo? $14. You’re not just saving money. You’re cutting the number of pills you have to take. Fewer pills mean fewer chances to miss a dose - and better health outcomes.
And it’s not just pills. Inhaled corticosteroid/LABA combos for COPD and asthma - like the Wixela Inhub example - show the same pattern. One device replaces two. One prescription replaces two. One co-pay replaces two.
How Much Are We Really Saving?
The numbers are staggering. According to the Association for Accessible Medicines, generic drugs saved $89.5 billion in the U.S. in 2023. That’s not just from switching from brand names. It’s also from switching between generics - and from choosing combinations over individual drugs.
Consider Crestor. Before generics, one pill cost $5.78. Today? $0.08. That’s a 99% drop. Prilosec went from $3.31 to $0.05. Again, 98% savings. But here’s the key: those savings didn’t happen overnight. They came from competition. When five companies started making the same generic, prices fell. When ten did, prices fell even more.
And when you combine that with combo products? The savings multiply. A 2023 study of the Mark Cuban Cost Plus Drug Company found that, on average, patients saved $4.96 per prescription. For uninsured patients? $6.08. That’s not pocket change. That’s enough to cover a month’s worth of co-pays for someone on multiple meds.
But here’s the catch: savings aren’t automatic. You have to ask for them.

How to Get These Savings - Step by Step
If you’re on multiple generics, or you’re paying more than you should for a combination drug, here’s what to do:
- Check your prescription list. Are you taking two or more pills that could be combined? Ask your doctor if a combo version exists.
- Ask your pharmacist: "Is there a cheaper generic version of this drug?" or "Is there a different strength or form that costs less?"
- Use the FDA’s Orange Book. It lists therapeutic equivalence ratings. Look for "A" ratings - those mean the generic can be swapped without losing effectiveness.
- Compare prices at different pharmacies. A 30-day supply might cost $15 at Walmart and $40 at your local pharmacy. Use GoodRx or SingleCare to find the lowest price.
- If you’re on Medicare or private insurance, ask your plan if they have a preferred generic combo on their formulary. If they do, they’ll cover it at the lowest cost.
Many people don’t know this: your pharmacist can often switch your prescription to a cheaper alternative without needing a new doctor’s note - as long as it’s therapeutically equivalent. You just have to ask.
Why Don’t More People Do This?
Because no one tells them. Pharmacies don’t always flag cheaper options. Doctors assume the prescribed generic is the cheapest. Insurance plans don’t always prioritize the lowest-cost combo. And patients? They’re just happy it’s "generic."
The system is designed for inertia. Once a prescription is written, it’s refilled - even if a better option exists. That’s why plan sponsors - like employers or Medicare - are being urged to audit their formularies quarterly. They need to remove high-cost generics and push the lower-cost alternatives.
But you don’t have to wait for them. You can take action today.

What’s Holding Back Bigger Savings?
There are still barriers. Some companies hold patents on delivery systems - like special inhalers or extended-release coatings - even after the active ingredient is off-patent. That lets them charge more. Others have consolidated: just 10 manufacturers control 40% of the U.S. generic market. Less competition means less price pressure.
And shortages are rising. The FDA recorded 258 generic drug shortages in 2022 - up from 166 in 2012. When a drug is in short supply, prices spike. That’s why it’s smart to have a backup option - like a different strength, form, or combo - ready to go.
The good news? The FDA approved 724 generic applications in 2023. More competition is coming. But it won’t fix everything. You still need to be your own advocate.
Real Savings, Real Impact
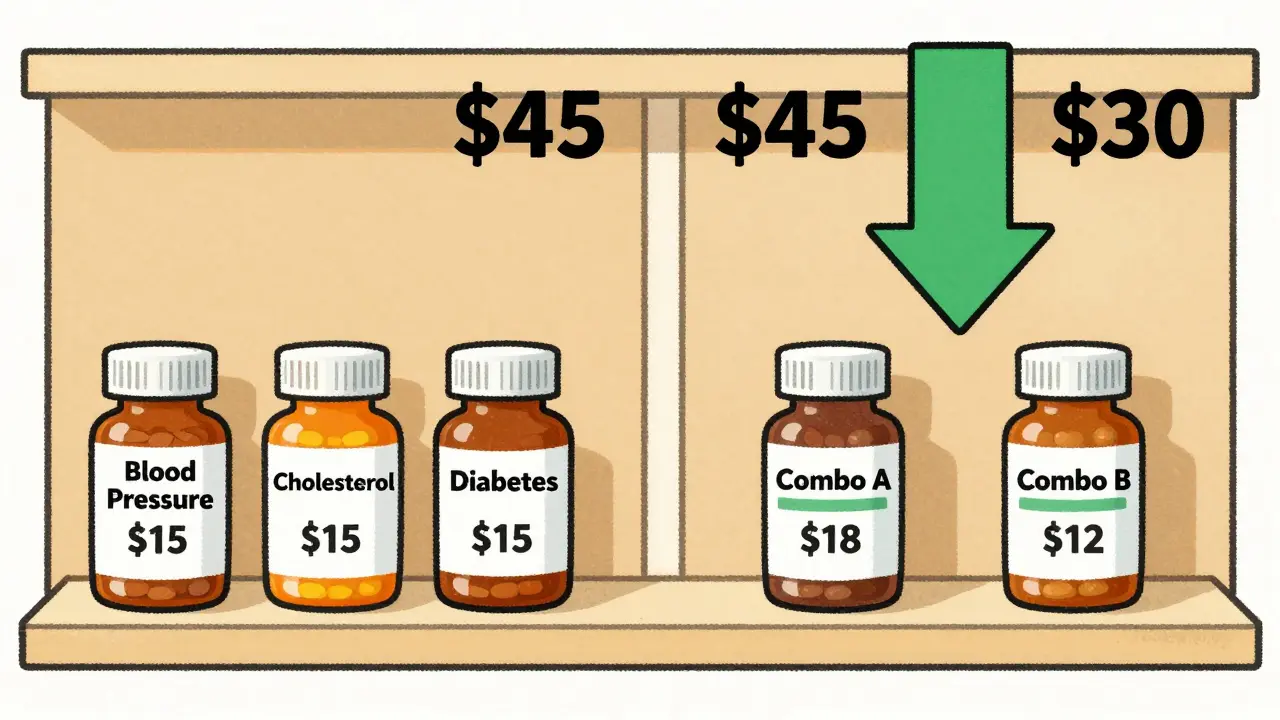
Imagine you’re on three separate generics: one for blood pressure, one for cholesterol, one for diabetes. Each costs $15 a month. That’s $45. Now imagine switching to two combo pills: one that combines blood pressure and cholesterol ($18), and one that includes the diabetes drug ($12). Total? $30. That’s $15 saved every month. $180 a year. Enough to cover a new pair of shoes, a weekend getaway, or a month’s worth of over-the-counter pain relief.
That’s not a stretch. That’s what’s happening right now. People are saving hundreds - sometimes thousands - a year just by asking the right questions. It’s not about switching brands. It’s about switching strategies.
The next time you refill a prescription, don’t just accept the price. Ask: "Is there a cheaper way to get the same medicine?"
Are combination generics always cheaper than buying individual generics?
Not always, but often. Combination generics are usually cheaper because they combine two or more drugs into one pill or inhaler, reducing manufacturing, packaging, and distribution costs. When multiple generic manufacturers compete to produce the combo, prices drop further. However, if only one company makes the combo, it might still be expensive. Always compare prices - sometimes buying individual generics separately is cheaper, especially if they’re from different manufacturers.
Can my pharmacist switch me to a cheaper generic without a new prescription?
Yes, in many cases. Pharmacists can substitute a generic drug for another if they have the same active ingredient, strength, and therapeutic equivalence rating (marked as "A" in the FDA’s Orange Book). This is called therapeutic substitution. You may need to give permission, but you don’t need a new doctor’s note - unless your prescription specifically says "dispense as written." Always ask your pharmacist if a cheaper option is available.
Why do some generic drugs cost more than others?
Generic drugs can vary in price because of competition. If only one company makes a generic, it can charge more. But if five or more companies make it, prices fall dramatically. Other factors include dosage form (capsules may cost more than tablets), packaging size (90-pill bottles are cheaper per pill than 30-pill bottles), and whether the drug has a patent on its delivery system (like a special inhaler). The FDA doesn’t regulate generic prices - only safety and effectiveness.
How can I find out if my medication has a cheaper alternative?
Start by asking your pharmacist. They can check the FDA’s Orange Book for therapeutic equivalents and compare prices across pharmacies. You can also use free tools like GoodRx, SingleCare, or Blink Health to see real-time prices. Look for different strengths, forms, or combo versions. For example, a 30-day supply might cost $20, but a 90-day supply could be $45 - that’s less per pill. Sometimes, switching from a tablet to a capsule or from a daily to a weekly dose can cut costs.
Do insurance plans encourage cheaper generic combinations?
Some do, some don’t. Insurance plans often have a "formulary" - a list of preferred drugs. If a combination generic is on that list, you’ll pay less. But if the plan hasn’t updated its list in a while, it might still favor an older, more expensive generic. Ask your plan if they have a preferred combo drug for your condition. If not, ask them to consider adding it. Many plans will change their formulary if enough patients request it.

Steven Pam
This is the kind of info that actually saves lives. I didn’t know combining meds could cut costs this hard. My mom’s on three separate pills for blood pressure and diabetes - switched her to a combo last month. She’s saving $40/month and actually remembers to take them now. Win-win.